CJC 1295 Weight Loss: Science & Results 2026
Losing fat is rarely just a math problem. Some people tighten nutrition, train consistently, and still feel like their body composition barely changes. That gap between effort and outcome is one reason cjc 1295 weight loss keeps showing up in research conversations.
CJC-1295 is a synthetic peptide studied for how it influences the body’s own growth hormone signaling. That matters because growth hormone and its downstream messenger, IGF-1, are tied to fat metabolism, recovery, and lean mass retention. Unfortunately, many articles fall short here. They blur research findings with treatment claims, skip the regulatory context, and ignore the populations where the evidence is weakest.
This article takes the slower, more useful route. It explains what CJC-1295 is, how it stimulates growth hormone release, what the current evidence suggests about fat loss, what researchers have observed in body recomposition settings, and where the actual limitations are. Throughout, the focus stays on research-only context, not consumer medical advice or human use recommendations.
Table of Contents
- Introduction
- How CJC 1295 Stimulates Growth Hormone Release
- Reviewing the Scientific Evidence for Fat Loss
- Observed Outcomes and Body Recomposition Effects
- Safety Profile and Adverse Effects in Studies
- Legal Status and Key Research Limitations
- Complementary Peptides in Metabolic Research
- Conclusion
Introduction
Most weight loss advice assumes the same starting point for everyone. Eat less, move more, stay consistent. That framework matters, but it doesn’t explain why some people struggle even when they’re doing the basics well.
Researchers became interested in CJC-1295 because it acts upstream of metabolism. Instead of directly supplying growth hormone, it’s studied as a growth hormone-releasing hormone analogue, meaning it signals the body to increase its own output through the normal control system. In plain language, it tries to influence the command signal rather than replacing the final hormone.
That distinction matters for people looking into cjc 1295 weight loss research. The interest isn’t only about scale weight. It’s about whether a compound can affect fat breakdown while helping preserve lean tissue, especially in settings where traditional calorie restriction often cuts both.
Practical rule: If a peptide article talks only about pounds lost and ignores lean mass, it’s leaving out the most important part of body composition research.
There’s also a more nuanced question that deserves attention. What about people with hormonally resistant or medication-related weight gain? Many popular guides treat all metabolic slowdowns as identical. The literature doesn’t support that assumption, and this article won’t pretend it does.
How CJC 1295 Stimulates Growth Hormone Release
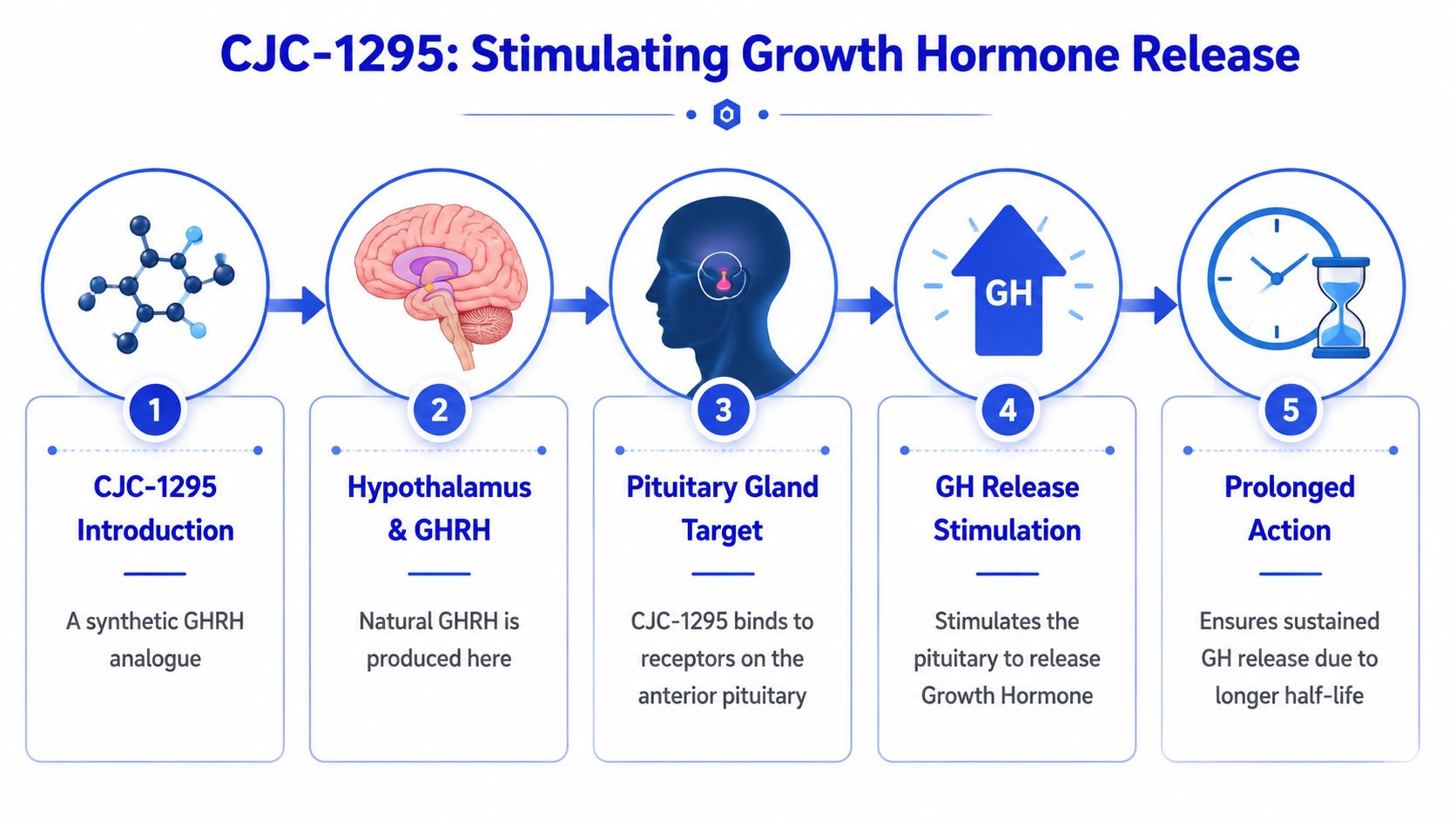
How can a research peptide influence body composition without supplying growth hormone directly? CJC-1295 is studied for that upstream role. It is a growth hormone-releasing hormone analogue, which means it is designed to imitate the signal that prompts the pituitary gland to release growth hormone through the body’s existing control system.
The mechanism becomes easier to follow if the pituitary is viewed as a regulated output center and GHRH as the signal that increases production for a limited period. CJC-1295 works like a longer-acting version of that signal. In research terms, the interest is not that it replaces growth hormone, but that it may prolong the instruction that tells the body to release more of its own hormone.
That distinction matters in metabolic research. A compound that changes signaling can produce different downstream effects than giving the end hormone from the outside, particularly when investigators are trying to understand body recomposition rather than simple water-weight changes.
What the human study showed
Human pharmacology research has reported sustained increases in circulating growth hormone and IGF-1 after CJC-1295 administration. For a reader new to endocrine signaling, IGF-1 can be understood as one of the main downstream messengers generated after growth hormone rises, with much of the longer metabolic effect passing through that second step.
Researchers often describe the sequence like this:
- CJC-1295 interacts with GHRH-related receptors
- The pituitary releases more growth hormone
- The liver responds by increasing IGF-1 production
- Tissues are exposed to a hormonal environment linked to lipolysis and lean mass maintenance
Often, confusion arises regarding this point. A higher growth hormone signal does not equal immediate fat loss. It means the body may shift toward a state that supports fat mobilization under the right study conditions, such as controlled nutrition, training, sleep, and baseline hormone status.
That last point is especially relevant for the under-discussed groups this article focuses on. In medication-induced weight gain or hormonally resistant weight gain, the question is not whether CJC-1295 can raise growth hormone in a healthy subject. The more difficult research question is whether that signal change is strong enough to matter when appetite regulation, insulin dynamics, sex hormones, cortisol patterns, or medication effects are already working against fat loss.
A useful analogy is a thermostat with a delayed furnace response. Raising the thermostat setting sends a clear instruction, but the final room temperature still depends on insulation, outdoor weather, and whether the heating system can respond normally. In the same way, increasing GHRH-related signaling may change the instruction sent to the endocrine system, but the visible body-composition result can vary sharply across populations.
So the central research idea is straightforward. CJC-1295 is studied as a way to influence the body’s own hormonal rhythm through a control signal. In a research-only context, that is a mechanism worth examining, not a guarantee of weight reduction.
Reviewing the Scientific Evidence for Fat Loss
The scientific case for fat loss doesn’t begin with dramatic before-and-after claims. It begins with mechanism. If a peptide raises growth hormone and IGF-1 in a sustained way, researchers then ask whether that shift changes how the body handles stored fat.

Why fat loss interest centers on visceral fat
The strongest research interest isn’t random fat loss. It’s visceral adipose tissue, the deeper abdominal fat associated with metabolic risk. In research discussions around CJC-1295 and related pathways, that’s a major reason the compound gets attention.
Clinical observations and patient reports involving CJC-1295 combined with Ipamorelin describe average weight loss of 5 to 12 pounds over 4 to 12 weeks with notable preservation of lean muscle mass, and visible fat loss is often reported between weeks 5 and 8, particularly in the abdominal area, according to studies. Those observations are useful, but they aren’t the same as large randomized outcome trials.
That distinction matters. Researchers can say the pathway is biologically plausible and supported by observations. They can’t say the evidence base is complete.
Why researchers compare this pathway with Tesamorelin
One of the best ways to understand the metabolic logic is by comparison. Direct large-scale trials on CJC-1295 for body composition remain limited, but peptides in this category are linked to fat loss through growth hormone elevation. A common reference point is Tesamorelin, an FDA-approved GHRH analogue used to reduce visceral fat in specific populations, which helps illustrate the therapeutic potential of this mechanism.
That doesn’t make CJC-1295 equivalent to Tesamorelin. It shows why scientists take the pathway seriously.
A short way to frame the evidence is this:
- Mechanistic support: GH and IGF-1 are tied to lipolysis and metabolic activity.
- Comparative support: A related GHRH analogue has an approved use tied to visceral fat reduction in a defined population.
- Observational support: Reports from peptide-focused weight management settings describe measurable fat loss with lean mass preservation.
- Limitation: Direct large-scale CJC-1295 body composition trials are still limited.
For readers who want a visual overview before going deeper, this video gives useful background on the broader discussion around peptide-driven body composition research.
Observed Outcomes and Body Recomposition Effects
Weight loss by itself isn’t always a win. If someone loses fat and muscle together, the scale may improve while metabolic resilience gets worse. That’s why researchers and coaches increasingly focus on body recomposition, not just body weight.
What body recomposition means in practice
In CJC-1295 research discussions, the interesting outcome is the combination of fat loss with lean mass support. Research summaries have highlighted approximately 10% increases in lean muscle mass over 6-month protocols, with that effect linked to IGF-1 driven protein synthesis pathways, according to this overview.
That doesn’t mean every research setting will produce the same result. It means the compound is being studied for a pattern that looks different from ordinary calorie restriction. Standard dieting often reduces both fat and lean mass. Peptide-based GH signaling research asks whether that tradeoff can be shifted.
Body recomposition is why scale weight can be misleading. A smaller waist with preserved muscle often tells you more than the number on the scale.
If you want a practical primer on how body fat and lean mass are measured, you can explore fitness with Zing Coach’s analysis. That resource is useful because it explains why two people at the same body weight can have very different metabolic profiles.
Timeline of observed effects in research cycles
Clinical observations described in the literature suggest a staggered timeline rather than a sudden transformation. Early effects tend to involve sleep, energy, and recovery. Visible body composition changes usually come later.
| Timeframe | Observed Effects |
|---|---|
| Weeks 1 to 2 | Initial improvements in sleep quality, energy, and recovery are commonly reported in observational settings |
| Weeks 5 to 8 | Visible fat loss and waist reduction are often observed |
| By 12 weeks | Body recomposition effects become more noticeable in reports involving CJC-1295 with Ipamorelin |
| Over 6 months | Research summaries describe lean mass gains and sustained body composition change in longer protocols |
That pattern helps explain a common misunderstanding. Some readers expect a peptide to behave like a stimulant or appetite suppressant. CJC-1295 research doesn’t fit that model. The changes are usually framed as gradual and tied to hormone signaling, recovery quality, and nutrient partitioning over time.
A reasonable interpretation is that researchers aren’t only chasing fat reduction. They’re studying whether the body handles energy differently when growth hormone signaling is modified in a sustained way.
Safety Profile and Adverse Effects in Studies
What should a careful reader look for in a peptide safety section. Not just whether adverse events occurred, but who was studied, how closely they were monitored, and how far the findings can reasonably be extended.

For CJC-1295, the published safety picture is still narrow. Early human research and observational discussion usually describe short-term tolerability in controlled settings, not broad real-world use across heterogeneous populations. That distinction matters because weight gain is not a single biological problem. A participant with uncomplicated obesity is different from someone with antipsychotic-associated weight gain, glucocorticoid exposure, thyroid dysfunction, polycystic ovarian features, or other hormonally resistant states.
What adverse effects were reported
Across the study settings most often cited in discussions of CJC-1295, the recurring adverse effects were relatively predictable. Injection site soreness or redness, transient headache, and flushing were the events described most often. In those controlled environments, investigators generally characterized these reactions as mild and self-limited.
That pattern suggests local irritation and short-lived vascular effects more than widespread systemic instability. A simple analogy helps here. The body can react to a peptide in two broad ways. It may respond at the point of administration, like skin becoming irritated after a vaccine or injection, or it may show broader endocrine disruption, such as meaningful shifts in blood pressure, glucose handling, or stress hormones. The available CJC-1295 literature discusses the first category more clearly than the second.
A restrained summary looks like this:
- Commonly described events: injection site soreness, redness, headache, flushing
- Typical severity in controlled studies: generally mild
- What appears less prominent in short-term reports: major acute instability in routine monitored measures
- What remains uncertain: long-term effects, repeat-cycle exposure, and outcomes in medically complex populations
The last point is the most important one for this article’s focus. Safety findings from healthy volunteers do not answer the harder question of how a growth hormone secretagogue behaves in people whose weight gain is driven by medication effects or endocrine resistance. Those groups may have different baseline risks, different co-medications, and different metabolic responses. In research terms, that is a gap in external validity. The study population may be too simple to stand in for the population many readers care about.
Why research context matters for dosing discussions
Requests for exact dosing protocols are common, but a paper’s protocol is part of an experiment, not a consumer instruction sheet. Researchers choose timing, monitoring, inclusion criteria, and stopping rules to answer a specific question under controlled conditions. Remove those guardrails and the meaning of the protocol changes.
That is why the research-only label is not a minor disclaimer. It defines the context in which CJC-1295 should be discussed. In laboratory or preclinical work, investigators care about identity, purity, storage conditions, batch consistency, and documentation because those factors affect whether results can be interpreted at all.
For laboratories evaluating materials, consistency and documentation matter as much as the compound itself. In that narrow research sense, Peptide Warehouse USA supplies CJC-1295 as a research chemical for laboratory, analytical, and preclinical applications, with third-party documentation such as COAs and related batch records described by the publisher.
A careful reading of the safety literature therefore leads to a modest conclusion. The short-term adverse effects reported in controlled study settings appear limited and mostly mild, but the evidence base is still too thin to make confident statements about long-term safety or about higher-uncertainty groups, especially those with medication-induced or hormonally resistant weight gain.
Legal Status and Key Research Limitations
The legal framing around CJC-1295 is not background noise. It shapes how the compound should be discussed, sourced, and interpreted.
Research chemical status is not a technicality
CJC-1295 is widely discussed in peptide circles, but it is not FDA-approved for general weight loss. In commercial settings, it is typically sold under a research-only label for laboratory, analytical, or preclinical use rather than human consumption.
That distinction protects against a common mistake. People often assume that because a mechanism looks promising, a compound has crossed the line into established treatment. It hasn’t. Research interest and regulatory approval are different categories.
A formal, evidence-based reading of the topic should keep three points separate:
- Mechanistic plausibility means the biology makes sense.
- Observed outcomes mean some studies and clinical settings report measurable changes.
- Regulatory approval would require a different standard of evidence for a specific indication.
The biggest blind spot in the weight loss discussion
The most overlooked issue isn’t whether CJC-1295 can affect growth hormone signaling. It’s whether that effect translates reliably in people with metabolically resistant or medication-induced weight gain.
A critical gap exists in the research for people with weight gain related to thyroid disorders, hormonal dysregulation, or medications such as corticosteroids, and existing content does not quantify outcomes for those populations.
That gap should change how readers interpret online success narratives. If someone has gained weight while taking medications that affect endocrine signaling, or if they have an underlying hormonal condition, there isn’t enough direct evidence to assume the same response seen in baseline populations. That doesn’t mean the peptide won’t matter in research. It means certainty would be false.
Complementary Peptides in Metabolic Research
CJC-1295 is rarely discussed in isolation. In metabolic research, investigators often compare or pair it with other peptide categories to see how different signaling routes affect body composition.
Why CJC-1295 is often paired with Ipamorelin
Ipamorelin is frequently studied alongside CJC-1295 because the two compounds act on related but distinct parts of the growth hormone release pathway. CJC-1295 is examined for its longer-lasting GHRH-type signaling, while Ipamorelin is studied as a selective ghrelin mimetic that supports growth hormone pulses without the same concern around disrupting cortisol or prolactin seen with less selective compounds in this class.
This pairing is one reason many discussions focus on recomposition rather than simple weight loss. Researchers are interested in whether combined signaling can support fat oxidation while preserving lean tissue.
How GLP-1 research differs
GLP-1 receptor agonist research follows a different logic. That category is usually discussed around appetite regulation, glucose handling, and energy intake, not growth hormone signaling.
For readers comparing approaches, the practical difference is straightforward:
- CJC-1295 research: studies hormonal signaling tied to GH and IGF-1
- GLP-1 research: studies appetite and metabolic regulation through a different receptor system
If you’re reading broadly on body composition protection during weight reduction, this guide on exercise for GLP-1 users adds useful context on preserving muscle while reducing fat mass.
Conclusion
CJC-1295 has earned attention in metabolic research because it targets a control point in the body’s own growth hormone system. The core idea is straightforward. A GHRH analogue may raise growth hormone signaling, increase IGF-1, and create conditions that support fat mobilization and lean mass preservation.
The available evidence supports scientific interest, not certainty. Human data show clear hormonal effects, observational reports describe measurable changes in body composition, and longer research discussions point toward lean mass preservation as a major reason this peptide stands apart from simple calorie-cutting strategies.
The most important caution is also the most ignored. CJC-1295 remains a research-only compound, and the literature has a real blind spot in populations with medication-related or hormonally resistant weight gain. If someone treats that unknown as settled science, they’re overstating the evidence.
For laboratories and institutions studying cjc 1295 weight loss, the useful question isn’t whether the topic is exciting. It’s whether the peptide is being evaluated with proper controls, realistic expectations, and clear sourcing documentation.
For laboratories and institutions conducting metabolic research, learn more about Peptide Warehouse USA to review its catalog of high-purity research peptides, including CJC-1295 formulations intended for laboratory, analytical, and preclinical use only.






Leave a comment